
Tennis Elbow: 5 Things You Should Know
April 3, 2017
A Simple Guide to Arthritis Surgery
May 31, 2017Musculoskeletal Ultrasound: Working for You
When patients come into our office suffering from an injury or chronic issue that requires imaging, we do our very best to keep the process non-invasive. That is, we try to make imaging choices that allow our patients to receive a diagnosis without having to schedule another appointment or visit a different facility. We are very aware that patients may be in pain and want immediate relief and don’t want to deal with the hassle or added expense of an MRI or CT scan. Plus, clients who are claustrophobic can suffer from severe anxiety during an MRI, which just makes the whole process of diagnosis that much more stressful.
There are many in-house tools we use as part of our diagnostic process, but one of our favorites is musculoskeletal ultrasound. This process is absolutely non-invasive and gives our doctors a clear view of many orthopaedic injuries.
What is Musculoskeletal Ultrasound?
Most people are familiar with ultrasound as a tool used during pregnancy, but its uses extend far beyond that purpose. Ultrasound is a non-invasive, painless procedure that uses high-frequency sound waves to produce an image of the inside of your body. It is especially good at providing medical professionals with a clear picture of what is going on with soft tissue issues in real time and at multiple angles, unlike x-rays that tend to show only clear images of bone, or MRIs that rely on a body remaining completely still during the procedure.
“Musculoskeletal ultrasound” is the term used when this technology is used specifically for diagnosing issues involving the muscles, ligaments, and tendons of the body.
Why is it Preferable to Other Imaging Methods?
When our doctors opt to use musculoskeletal ultrasound technology, it’s usually as the first step in imaging depending on the type of issue a patient presents on their visit. When making decisions about how to diagnose a problem, we keep the patient’s comfort and overall well-being in mind, including being wary of procedures that could expose patients to unnecessary radiation, expense, or distress. If there is no reason to send a patient for a more invasive, more expensive procedure, we will avoid doing so.
Ultrasound does a fantastic job of creating a close-up image of soft tissue injuries. Unlike procedures such as MRIs, CTs, and X-rays, ultrasound allows medical professionals to move the body during the process and immediately detect problems from a different viewing angle. Minuscule tendons and nerves are not an issue for the ultrasound, which helps the doctor visualize the exact location of problems and what changes an injury or chronic condition may cause. The doctor can also see real-time blood flow, allowing the identification of problem areas quickly and providing insight on what may be happening to cause the patient’s discomfort and how to best provide relief.
When is it Likely to Be Used as Part of a Visit?
Ultrasound imaging has a wealth of applications. It can be implemented in a variety of ways to help patients receive a clearer diagnosis of injuries, as well as a better picture of the severity of chronic issues such as carpal tunnel syndrome. The examining physician decides whether or not to use the ultrasound as part of a visit based on the patient’s symptoms, the location of the problem, and the probability of the results providing enough information to negate the need for additional imaging.
We also use this technology in our practice during some injection treatments. Ultrasounds do an excellent job of showing medical professionals exactly where a needle needs to be placed in relation to treatment areas, ensuring that the patient receives the most benefit from the injection.
What to Expect From This Procedure
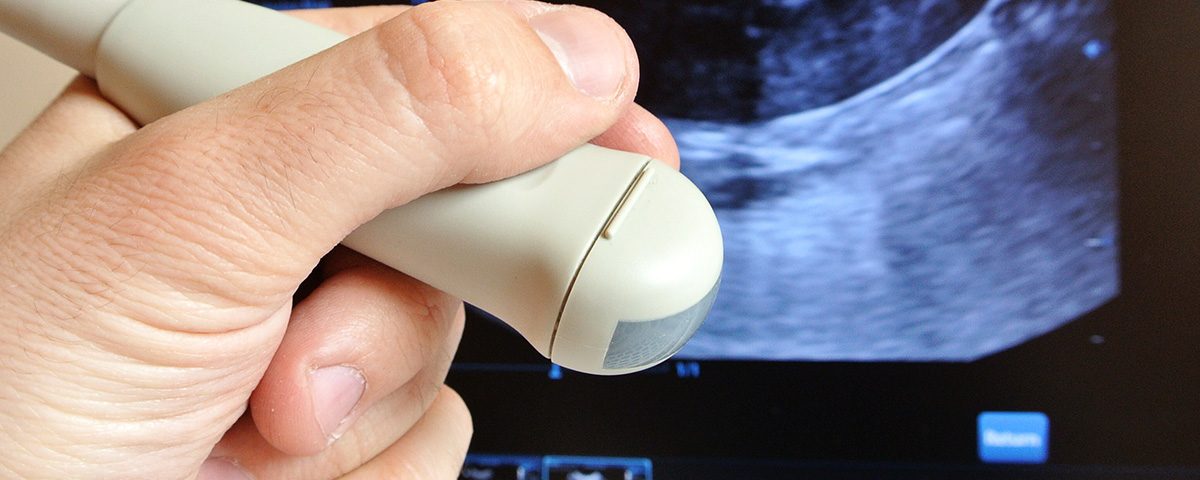
Patients receiving an ultrasound as part of their diagnosis have no reason to be concerned about pain or recovery time – it is one of the easiest medical procedures to undergo. To create an image, the person administering the ultrasound will squeeze a bit of gel on the affected area and then press the ultrasound wand to the patient’s skin. An image of the affected area will then appear on a screen. There may be some pressure and slight discomfort if an injured area is painful to the touch and the person administering the ultrasound needs to move the wand around to get a better look. Interpretation of the image happens in real-time and, unlike other imaging technologies, does not expose the patient to any radiation.
The whole process takes about 30 minutes. For some injuries or chronic issues, multiple ultrasounds may be necessary to track the healing process or to assess the success of treatments. It’s an easy and accessible process that can make a big difference to those suffering from orthopaedic-related pain!



